Intraabdominal hypertension in a patient with neutropenic enterocolitis – an absolute contraindication for surgery?
Written by Joël Lavanchy
Category
Published 20 December 2017

Intraabdominal hypertension in a patient with neutropenic enterocolitis – an absolute contraindication for surgery?
Joël Lavanchy MD, Tobias Haltmeier MD, Beat Schnüriger MD
Department of Visceral Surgery and Medicine, Division of Acute Care Surgery, Inselspital, Bern University Hospital, Bern, Switzerland
Case
A 63-years old male patient has been referred to our hospital with fatigue since 3 months, shivering without fever for 6 days and dry cough that started 3 days ago. Suspecting pneumonia, the general practitioner started an antibiotic treatment with Co-Amoxicillin the day before hospital referral.
At admission, the patient presented in a hemodynamically stable but febrile state. Laboratory findings revealed pancytopenia with 58% blast cells. Acute myelogenous leukemia was diagnosed by bone marrow aspiration. The patient was transferred to the oncological ward. At hospital day 4 induction chemotherapy with Cytarabine and Idarubicin was started. Two days later the patient was in aplasia (Fig. 1).
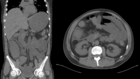
Later in the clinical course the patient developed abdominal pain and diarrhea. Abdominal computed tomography (CT) showed neutropenic colitis of the ascending colon (Fig. 2).
On day 17 after admission the patients’ general condition deteriorated and he developed septic shock. He was subsequently transferred to the intensive care unit, underwent tracheal intubation and was resuscitated with crystalloids, high-dose vasopressors, and empiric broad-spectrum antibiotic therapy.
However, hemodynamic stabilization was not achieved. Moreover, the patient developed intraabdominal hypertension, that did not respond to conservative measures (muscle relaxation, sedation).
After an interdisciplinary discussion of the therapeutic options taking into account the aplasia and careful consideration of the patient’s presumed will with his family, emergent exploratory laparotomy was conducted. Intraoperatively the colon presented diffusely inflamed with thickening of the bowel wall. The fascia was left open and an abdominal negative pressure wound dressing was applied. Planed 2nd look laparotomy was performed on the second postoperative day. No mesenteric ischemia was found. The abdomen was closed with an inlay mesh placed over the abdominal negative pressure wound closing system (vacuum-assisted wound closure and mesh-mediated fascial traction technique)1. On postoperative day 5, intraperitoneal onlay mesh placement (IPOM) and fascial closure were performed.
Filgastrim (G-CSF) was administered from postoperative day 3 to 8. Normalization of the neutrophil count was observed seven days after surgery. On hospital day 35 the patient was transferred to the regular ward. Two weeks later he was transferred to a rehabilitation center.
Discussion
Neutropenic enterocolitis may occur as an infectious complication in patients with severe neutropenia2, 3. Most frequently the cecum is affected. It was first described in children with induction chemotherapy for acute leukemia and was later described in immunosuppressed patients for different reasons (e.g. lymphoma, AIDS, immunosuppressive medication). An inflammatory damage to the mucosal barrier with subsequent translocation of microorganisms is a possible explanation for the development of neutropenic enterocolitis4. However, the specific pathophysiologic mechanisms are not fully understood. The true incidence of neutropenic enterocolitis is largely unknown. Incidence rates vary from 3.5% to 5.3% in patients hospitalized for treatment of hematological or solid malignancies and drug induced aplasia5, 6. There is no high-level evidence regarding treatment strategies of neutropenic enterocolitis. Two systematic reviews suggest conservative treatment with fluid resuscitation, bowel rest, nasogastric tube insertion, total parenteral nutrition and broad-spectrum antibiotics7, 8. A European guideline advocates the use G-CSF in patients with a high-risk of febrile neutropenia9. Thirty-year old case series have proposed surgical management in patients with neutropenic enterocolitis and hemorrhage, free intraperitoneal perforation, and shock not responsive to conservative management2, 10, 11. However, there are no clinical studies investigating this topic and no recent case series.
Conclusion
There is a great uncertainty when dealing with patients in aplasia and acute disease that may require surgical intervention. Conservative treatment is recommended due to the severe immunosuppression that may lead to infectious complications and compromised wound healing in these patients. However, after careful consideration and interdisciplinary discussion of the therapeutic options, surgical intervention may be indicated.
What is your opinion? Would you perform laparotomy in a patient in aplasia? Please leave your comment below (only logged-in SwissACS members).
References
1. Petersson U, Acosta S, Bjorck M. Vacuum-assisted wound closure and mesh-mediated fascial traction--a novel technique for late closure of the open abdomen. World J Surg, 2007;31:2133-7.
2. Shamberger RC, Weinstein HJ, Delorey MJ, Levey RH. The medical and surgical management of typhlitis in children with acute nonlymphocytic (myelogenous) leukemia. Cancer, 1986;57:603-9.
3. Amromin GD, Solomon RD. Necrotizing enteropathy: a complication of treated leukemia or lymphoma patients. JAMA, 1962;182:23-9.
4. Urbach DR, Rotstein OD. Typhlitis. Can J Surg, 1999;42:415-9.
5. Gorschluter M, Mey U, Strehl J, et al. Neutropenic enterocolitis in adults: systematic analysis of evidence quality. Eur J Haematol, 2005;75:1-13.
6. Aksoy DY, Tanriover MD, Uzun O, et al. Diarrhea in neutropenic patients: a prospective cohort study with emphasis on neutropenic enterocolitis. Ann Oncol, 2007;18:183-9.
7. Davila ML. Neutropenic enterocolitis. Curr Treat Options Gastroenterol, 2006;9:249-55.
8. Rodrigues FG, Dasilva G, Wexner SD. Neutropenic enterocolitis. World J Gastroenterol, 2017;23:42-7.
9. Aapro MS, Bohlius J, Cameron DA, et al. 2010 update of EORTC guidelines for the use of granulocyte-colony stimulating factor to reduce the incidence of chemotherapy-induced febrile neutropenia in adult patients with lymphoproliferative disorders and solid tumours. Eur J Cancer, 2011;47:8-32.
10. Alt B, Glass NR, Sollinger H. Neutropenic enterocolitis in adults. Review of the literature and assessment of surgical intervention. Am J Surg, 1985;149:405-8.
11. Moir CR, Scudamore CH, Benny WB. Typhlitis: selective surgical management. Am J Surg, 1986;151:563-6.

Do you have similar patients undergoing acute care surgery in aplasia? We are very interested in your experiences when dealing with these patients.